Virtual Diabetes Center
The Virtual Diabetes Center (VDC), developed by the Diabetes Task Force Solutions team, addresses gaps in the current delivery of chronic-diseases care. This includes the growing imbalance between the number of patients with diabetes and the number of healthcare providers, access to care, and patient education and motivation; in addition to the necessary enhancement of the overall efficiency of diabetes-care work-flow and health outcomes by adopting a proactive approach to type 2 diabetes treatment and care.
The proactive approach starts with knowledgeable and motivated patients who are active partners in managing their diabetes, rather than being passive recipients of care. Diabetes self-management data: diet, physical activity, sleep, stress, allergies, social activities and environmental factors are essential to understanding what affects a patient's blood sugar control. Such data are also indicators of preventive actions. Continuous monitoring, as well as access to care by multidisciplinary healthcare providers, are also key to early intervention.
VDC consists of four separate Cloud-based applications. Each function as an independent application or as an integrated solution to provide complete diabetes-care solution based on your requirements. These are Diabetes Case Management, Patients Health Management, Patient Diabetes Self-Education and Continuing Medical Education.



The proactive approach starts with knowledgeable and motivated patients who are active partners in managing their diabetes, rather than being passive recipients of care. Diabetes self-management data: diet, physical activity, sleep, stress, allergies, social activities and environmental factors are essential to understanding what affects a patient's blood sugar control. Such data are also indicators of preventive actions. Continuous monitoring, as well as access to care by multidisciplinary healthcare providers, are also key to early intervention.
VDC consists of four separate Cloud-based applications. Each function as an independent application or as an integrated solution to provide complete diabetes-care solution based on your requirements. These are Diabetes Case Management, Patients Health Management, Patient Diabetes Self-Education and Continuing Medical Education.
Patient Education

Patient Self-Management

Diabetes Case Management

Continuing Medical Education

VDC is a proprietary digital health ecosystem for diabetes and other chronic diseases management; it facilitates the collaboration between healthcare providers,
and Integrates patients' self-management and lifestyle data with current health conditions and historical medical records. Utilizing proprietary automated algorithms,
VDC organizes and provides such information in easy-to-review visuals, giving healthcare team members a comprehensive understanding of the relation between patients' lifestyle, their diabetes management, and the current prescribed treatment,
all which is essential for successful management of chronic diseases and improved health outcomes.
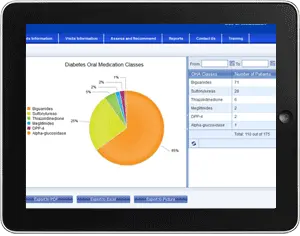
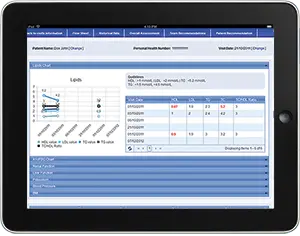
VDC generates comprehensive medical reports, decision support based on clinical guidelines, and risk analysis for type 2 diabetes, CKD, and CVD. VDC's provide comprehensive analytics tools, a series of standardized reports and customizable queries for outcome analysis. Healthcare professionals and administrators can quickly and easily generate statistics regarding patients' clinic, medications and laboratory results, and treatment outcome using similarity analysis. These statistics and reports can be converted to PDFs and exported into Excel for integration into medical papers or for other uses. The program can also develop a recall list. Patients who have high indicators can receive automated notifications to see their healthcare team.
VDC integration in the diabetes care work-flow

|
Education and Motivation - Following the diagnosis by the family physician (or already diagnosed), patients are advised to start learning about diabetes through an authenticated web-based diabetes education portal prior to attending educational classes at Diabetes Education Centres. The Virtual Diabetes Center's Patient Education Portal is currently used by the British Columbia Endocrine Research Foundation (BCERF) for its Live Well with Diabetes initiative. This program provides culturally sensitive education in nine languages.
Patients are also referred to a local pharmacy to learn about monitoring and injection devices and as well as any prescribed medication. They are also referred to the local Diabetes Education Centre. |
|
Self-Management - Patients are provided access to the Virtual Diabetes Centre's Patient Self-Management Recording application.
Patients must be encouraged by their healthcare provider to monitor and record their blood sugar levels and lifestyle factors to understand how to manage their diabetes. This information is vital to train the patient on managing diabetes, and recommended lifestyle changes (with the support of other care team members including registered dietitians, social workers, physical trainers, etc.), as well as for physicians to prescribe accurate treatment.
Patients can record self-management data manually or by using wearable that are accessible by the application through APIs. |

|
Examination and Motivational Interviewing - Prior to the doctor's visit and following a group education session, a one-on-one motivational interview with a diabetes nurse educator (case manager) or a pharmacist with diabetes education certification will allow the patient to address specific concerns and review self-management records.
The nurse or pharmacist will use a diabetes medical records system to record a patient's current health conditions, family history and other health complications. |
|
Specialists' Consultation - VDC generates a comprehensive medical report that can be sent to a diabetes specialist as required. Diabetes specialist can remotely access VDC to provide additional recommendations or request to see the patient if required.
Virtual Care - Virtual care will be provided through VDC's secure message and video chat tools. Nurses, pharmacists, and family physicians could communicate with the patients regarding specific questions. |

|
Analytics - VDC provide analytics tools that includes a series of standardized reports and customizable queries for outcome analysis. From the database, the healthcare team quickly and easily generates statistics regarding patients' clinic, medications and laboratory results. These statistics and reports can be converted to PDFs and exported into Excel for integration into medical papers or for other uses. The program can also be used to develop a recall list. Patients who have high indicators can receive automated notifications to see their healthcare team. |
Diabetes Proactive Care Road map
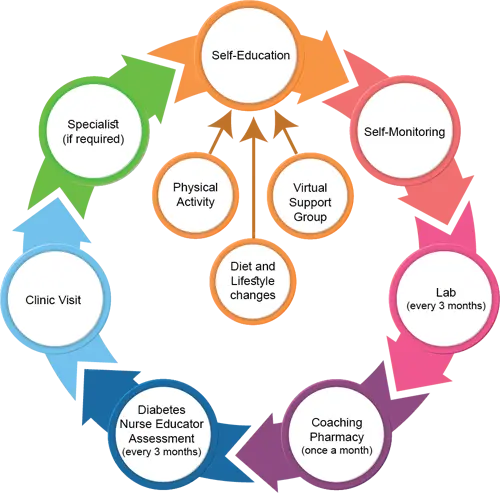
VDC Automated Tools forPatients Care
|
Virtual Diabetes Center provides
- Personalized patient education and motivation
- Continuous monitoring and support via video, text chat, and social media (peer support)
- Visualization of current and historical clinical data, and patient self-management data in easy-to-review visuals to maximize the use of patients' visit and more accurately diagnose and treatment
- Algorithms for decision support and treatment (AI) based on clinical guidelines and cases similarity analysis.
- Comprehensive medical reports with data visualization
- Efficient collaborative care and patient engagement
- Virtual access to specialists
- Cost saving and efficiency of diabetes care work-flow

Working together to improve diabetes care
Contact us
